Three little letters that mean so much to a patient: PRN. It’s a term often used but poorly understood. We see it on prescription bottles. We look at it but we just glance over it.
What is PRN? It stands for ‘pro re nata’, a Latin phrase meaning “as the circumstance arises”. PRN in practical terms means the patient has the liberty of taking medication as needed, without adhering to a strict schedule. It gives patients control over when and how they take their medications.
But control is a funny thing in healthcare, as autonomy can quickly convert to liability. Ostensibly, when patients are given prescription orders written as PRN, it implies patients can regulate when to take their medication; that patients understand the relationship between their symptoms and the medications prescribed to treat those symptoms.
But lately, health regulators have strained that relationship for chronic pain patients through a host of administrative oversights, particularly prescription databases and urine drug screens.
Known as PDMP’s or prescription drug monitoring program (PDMP), these databases track controlled substance prescriptions per patient and per provider. It monitors when prescriptions are written, when they are filled – or ‘sold’ as the database insists on phrasing it – and at which pharmacy they are filled. It ensures prescribed opioids are used for their intended medical purpose by the patient it was prescribed to. At least that’s the intention.
But it doesn’t account for those three little letters: PRN. And for chronic pain patients, the PRN distinction creates a frightening disconnect between how medications like opioids are used and how they are monitored.
Rather than take opioids as the circumstance arises, namely whenever patients experience pain, many chronic pain patients resort to enduring bouts of intractable pain to ensure they have enough medications to last the duration required in the PDMP databases – even when they experience intense flares of pain.
Though these events are known to occur among chronic pain patients and represent true medical need – hence using the term, ‘PRN’ – they raise the proverbial red flag of those monitoring the prescription databases. Now, when patients experience these exacerbations, they no longer feel empowered to take medications as they see fit. Instead, they see their medication use as a liability.
The mere speculation of clinical consequences that can arise if they fail to meet the monitoring standards of a PDMP database leaves patients in a compromised state of mind. They remain mired in uncertainty, perpetually rehashing an ongoing Faustian negotiation between treating their pain and monitoring their pill count.
Should they fall short, perhaps by succumbing to a slew of pain exacerbations, they may find themselves at the mercy of another instrument of administrative oversight, the urine drug screen. If providers find no opioid or opioid derivative in the urine test, then they accuse the patient of diverting medications, regardless of the number of pain exacerbations. The PRN distinction no longer applies, gone in favor of the tyranny of oversight.
Do the dates between prescription orders match up?
Does the urine drug screen check out?
If either of the questions is answered unfavorably, regardless of the reason, then the patient is stigmatized, labeled, and forced to undergo a slew of punitive measures in the name of diversion control: forced tapering, terminating the patient contract, or even abandoning the patient on the spot. God forbid a provider incurs legal liability in addressing a patient’s medical needs.
The patient-provider relationship is no longer about a symptom and a medication, but between medical need and medical oversight: Two components that should align, but are increasingly at odds.
It makes the PRN distinction a distinct liability for patients who were once in control of managing their pain, who are now at the mercy of a merciless system of oversight – comprising prescription databases and urine drug screens – ever vigilantly monitoring patients to ensure they have enough medications to last until their next appointment.
Patients respond by storing extra medications – just in case. It’s human nature. Our ancestors kept excess food supplies for times of famine. And today, pain patients keep extra quantities of opioids to address pain exacerbations. This is not an isolated phenomenon relegated to fringe patient populations teetering on the verge of dependency. It’s far more common than we like to admit. A study on post-operative opioid use found 83% reported taking half or less of the prescribed opioids following their hospital discharge.
It means a high percent of patients have extra opioids leftover. Normally this would be disposed of or returned to the provider, but for chronic pain patients, the uncertainty of not knowing whether they will receive their pain medications leads them to prepare for worst-case scenarios.
Eventually, those few extra opioids become a hoard of pills. And the risk of diversion the system of oversight intends to protect against creates an even greater risk diversion from patients keeping a surplus of opioids at their place of residence. Which, by most patients’ accounts, are stored in an unlocked bathroom cabinet or a common area medicine cabinet – locations easily identifiable for those seeking to abuse opioids.
The more patients fear the consequences of excessive oversight, the more they are willing to store their own supply of opioids; and the more opioids available in the patients’ residence, the greater the risk of abuse.
Welcome to the opioid epidemic, where irrational policy leads to obvious moral hazards.















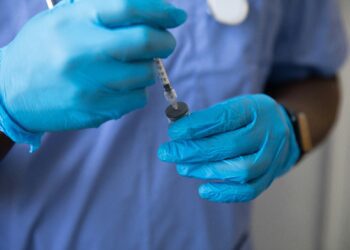
Occasional “hoarding” of pain meds isn’t going away for reasons stated in the article.
Perhaps patients could be educated about potential diversion and ways to avoid it. For example, keeping their extra pain meds in a safe or locked location.