Dr. Xiulu Ruan has eight board certifications, a world record. He was the first physician trained as a Physiatrist who was recruited to be an Interventional Pain Fellow at the University of Michigan Health System. He ran a prolific private-practice focusing on pain management in Mobile, AL, serving nearly 8,000 patients.
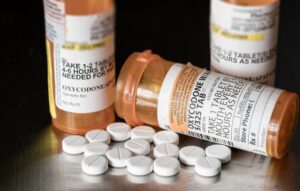
He is now in federal prison, sentenced to 21 years for allegedly prescribing opioids illegally. Only there was no overt criminal act that landed him in his current lot. Rather, it was the absence of what non-clinically trained federal prosecutors believed to proper oversight. And when Dr. Ruan attempted to defend his actions as those performed in the best interests of patients, in good faith, the Eleventh Circuit federal court system – both district and circuit courts – denied the allowance of such a defense.
He now finds himself in front of the Supreme Court, the highest court in the land, arguing whether he should be allowed a defense that most would consider obvious – can a physician be criminally charged for clinical behavior performed in good faith?

Most would consider the answer a straightforward no and the case simple enough to not require the high court’s time. But the opioid epidemic is anything but straightforward or simple. And the ensuing implications of a ruling in favor of Dr. Ruan will reverberate far beyond the original intent of the question – through the entire opioid epidemic and all the layers of policy and laws designed to curtail opioid abuse.
The question, like most things at the intersection of healthcare and law, appears simple enough, but is insidiously complicated. Good faith, as it is defined in the Controlled Substance Act, the law used to indict and convict Dr. Ruan, is a poorly constructed term, defined through vague, clinically irrelevant wording.
It is precisely through these ambiguities that the term good faith has been manipulated to represent anything but its original intent. Now it is understood through a legal interpretation of clinical behavior, defined by federal prosecutors who presume that by reducing opioid prescriptions, we will reduce the number of opioid related mortality.
But in heeding such misguided notions, federal prosecutors have similarly misinterpreted the definition of good faith, to one that is outside of its medically appropriate meaning. Good faith is not just a characterization of a singular action, but of one clinical action relative to another, to be examined within a broader context of patient care.
To understand this, we must begin where most physicians start their careers – by pledging an oath to patients. Most nascent physicians swear upon either the Hippocratic Oath or the Oath of Maimonides. In the latter, there is a distinct line that encapsulates a requirement for all physicians:
“May I never see in the patient anything but a fellow creature in pain.”
It implies that a physician by nature must implicitly trust patients unless proven otherwise. But trust cannot be afforded blindly; it must be balanced with oversight. Good faith is defined through the series of clinical actions within the context of a patient encounter that forms this balance.
For example, although access to care must be the default course of action for any physician, that access must be balanced with oversight, whether that is urine drug screens, imaging studies, or a review of a patient’s prescription history.
Law enforcement, not versed in pain management or addiction medicine, simply views the prescribing of opioids as a drug deal exchange. This is why prosecutors focused less on clinical decision-making and more on specific acts, or purported red flags, that inductively insinuate a physician behaved in a criminal manner with criminal intent.
Clinically, it has been proven that access to care improves quality of care. Instead of simply cutting off patients from medically necessary medications and incurring patient harm in the process, healthcare providers must continue to provide access to patient care while addressing the risks of abuse.
Access to healthcare is the essence of healthcare. The very concept of emergency care ensures access to care for all patients at all hours. Should every patient who presents to the emergency room with pain be denied medications unless they have legal verification to justify a prescription for opioids?
When we clarify the definition of good faith, we are actually clarifying the balance between access to care with its oversight – which translates into the courts as a comparative analysis of two legal interpretations – that of good faith with mens rea.
Mens rea is, true to topic, also a complex concept and derived from common law. It requires that the accused demonstrate criminal intent in order to be convicted of a particular crime, which modern courts have distilled into four component classifications.
-
1. Acting purposely – the defendant had an underlying conscious object to act
-
2. Acting knowingly – the defendant is practically certain that the conduct will cause a particular result
-
3. Acting recklessly – the defendant consciously disregarded a substantial and unjustified risk
-
4. Acting negligently – the defendant was not aware of the risk, but should have been aware of the risk
When applied to most modern criminal cases, mens rea appears in one of two ways. The first is when a defendant commits an act knowing it is criminal in nature or has criminal consequences. The second is when a defendant does not commit an act, either knowing the lack of action will result in a criminal consequence or recklessly disregarding knowledge that he or she should have had.
Most healthcare crimes pertaining to the improper prescribing of opioid analgesics during the opioid epidemic are prosecuted the second way, where a prosecutor attempts to show that the lack of action, or the blatant disregard of oversight on the part of the physician, was criminal.
However, without the requisite clinical understanding, law enforcement often distorts or retroactively reinterprets particular actions or the absence of actions as criminal – because they do not balance access to care with oversight.
Effectively, when we conflate specific actions, or the lack thereof, as representative of clinical behaviors in its entirety, we are erroneously conflating isolated behaviors as representative of mens rea.
This is nothing more than conflating individual actions with broad definitions and misguided logic for healthcare experiences. Through such erroneous thinking, the potential risk of diversion has superseded the actual risk of poor clinical care.
Healthcare and law interact in its own balance, which balances the experience of healthcare with the logic of clinical decision-making, the primary clinical risks with the secondary and tertiary clinical consequences, and the quality of care with the socioeconomic constraints limiting it.
But among the many ways this complex balance can be viewed, we must recognize that the experience of healthcare is paramount – more specifically, the experience of those most vulnerable to misinterpretations or interpretive abuses of healthcare law.
And through this balance, we can clarify the definition of good faith – recognizing violations of good faith based on the relative balance of actions and behaviors perceived to be in good faith, relative to those perceived to arise out of mens rea.
Such a balance recognizes the difference between a medical error and a violation of personal liberty, differentiating between the two primarily through the patient experience.
But when law is subject to the whims of novel and medically inappropriate interpretations, the definition of good faith changes based on the interpretation presented. Over time these changes lead to ever weakening legal arguments. Eventually inductive logic and circular reasoning justify any crime. Soon even a well-intentioned medical error, transpiring over the course of clinical care, becomes a crime.
Yet healthcare needs error. In fact, medical errors are critical to healthcare, necessary for its advancement – errors form the basis of experimentation, which forms the basis of clinical research.
Instead of allowing healthcare to regulate itself, advancing through natural errors, the government has begun to regulate healthcare, which has changed the perception of medical errors. Errors are no longer seen as a natural part of healthcare but as willful acts of criminal transgression. Now instead of legal arguments based on medical data, we see subjective interpretations of clinical behavior absent the clinical context when describing medical errors.
All clinical care is founded upon the principle of good faith, which forms the essence of a trusting relationship between physicians and patients. Any perceived violation of good faith must first balance good faith with mens rea by evaluating the totality of actions and decisions from the perspective of the patient experience. And then proceed to analyze the many attributes that form the complex balance of clinical decision-making and patient care – relative to one another.
If we think of healthcare and law as a balance, then the distinction between errors and crimes and the complex balance between good faith and mens rea becomes more discernible.
It is when we define healthcare behavior in absolute terms absent any clinical context that errors become crimes – creating contradictions between justice and freedom. As the French novelist Albert Camus wrote, “absolute justice is achieved by the suppression of all contradiction: therefore it destroys freedom.”

















GET THE FEDS
OUT OF MEDS!
Since when did DEA police (Gestapo) and DOJ prosecutors (Reichstag) attend Medical School? What & Who gave these Cold Turkeys and OxyMORONs – whose LACK OF KNOWLEDGE of NEUROLOGY, ANATOMY, PHYSIOLOGY, PHARMACOLOGY, PAINCARE MEDICINE, DENTAL PAIN, POSTOP PAIN, PEDIATRIC PAIN, INJURY PAIN, LIFE-LONG CHRONIC PAIN – should prevent these criminal interferers in healthcare from raiding doctors’ practices, seizing assets/patient records, killing doctors’ careers…ultimately, pain patients suiciding, a PAINDEMIC, and even some targeted MDs suiciding when imprisoned by federal persecutors <-ignorant of quality medical care for patients in pain. This KINDERGARTEN APPROACH, MANHANDLING OPIOID-PRESCRIBING CLINICIANS THUS LEAVING PAIN PATIENTS IN EXTREMIS (unable to keep their jobs or interact with family, rendering them bedridden when, on their Rx opioid they could work and participate in life) robbed of their appropriate opiate or opioid prescriptions is a crime, by our federal government that needs to be prosecuted by Congress. Meantime, these same gov't criminals are incapable of deterring, jailing and prosecuting dealers of illicits that are poisoning addicts. These PERSECUTIONS OF PHYSICIANS TAKING PROPER CARE OF THEIR PAIN PATIENTS IS A BLOODSTAIN ON AMERICA AND MUST CEASE IMMEDIATELY….and gov't microcephalics perpetrating these horrific prosecutions and jailings MUST BE HELD ACCOUNTABLE AND PUBLICLY SCORNED! Helen Borel,RN,MFA,PhD, Writer of "AMERICAN AGONY: THE OPIOID WAR AGAINST PATIENTS IN PAIN"
>. But the opioid epidemic is anything but straightforward or simple.
The opiod crisis is not about prescription drugs. It is about a massive influx of cheap black market Chinese Fentanyl analogues of unpredictable strength & a lot of cheap heroin – which began flooding over the US southern border some time ago. It hit other parts of the world too but not to the extent it hit the UA.
Fentanyl was in the USA for several years in poor non-white communities being ignored by cops and government and then that black market Fentanyl from China found it’s way into predominantly white suburbs. For a couple of years a lot of upper middle class white people who did recreational narcotics had overdoses because they kept getting Fentanyl analogues in what they thought was heroin. Most of them lived but far from all. By the time the press started talking about this the rates of overdoses had been falling for about 2 years (as usual late to the game).
The OTHER thing which is NOT the opioid/opiate crisis is about a few pharmaceutical companies whose sale reps set up special kickback deals with clinics in US states where pill mills have existed for ages. It was not a new thing. It was not everywhere.
The idea that there were huge numbers of opioid/opiate addicted people all over the USA is utter bullshit. The concept that people were becoming addicts from pain medication given after surgery or some injury is not based in fact. The interviews on TV weren’t at all credible. The reports that people were dying in large numbers from being given pills from their doctors was not at all factual. The two CDC papers that supported this (claiming that people became addicts and died of overdoses from very small doses of medication after surgery) were destroyed in peer review and removed from publication *forcably*.
You would know all of this if you read sources other than the yellow press who have had this wrong from the start. Murdoch has a lot of answer for here. In fact the press as a whole has been horrible on this topic because it’s easy to believe anything bad said about drugs. It’s confirmation bias. As a result the press has constantly conflated a flood of black market narcotics over the southern border with the same old pill-mill and kickback scams that have been around in those US states for ages.
Conflating these two things and echoing claims backed by nothing but hysteria has created a moral panic (opiod hysteria) that has doctors refusing to treat and states forcing docs to not prescribe. As a result a lot of people in agony are committing suicide or turning to street drugs to try not to die. All those people are in that situation because of really irresponsible reporters using the War on Drugs to advance their careers – and because there is so much power to be had from fear.
I suggest you actually read about a topic before posting on it. You obviously did not do so in this case.
I’ve had severe pain issues for years, and I don’t even try to quantify it to someone else because I simply can’t. I was on opioid pain medications for years and I led an actual life. I could get out almost like anyone else, and the difference between how I felt then and how I feel now is incalculable. They weren’t magic, and they didn’t fix everything, but again the difference they made was absolutely phenomenal, and I can say that now with neither doubt nor reservation roughly three years after being unable to access pain management that utilizes opioids – and I’ve tried everything. I still do, some conventional, some not so much, but the fact is that now, for all intents and purposes all I am doing is pretty much killing time until I die, and that’s sad and it sucks. As far as what someone else thinks of what I do, or what I consume, I could give two $hits. I’ll do me, and they can do them. Of course, I don’t blame doctors….not at all. I feel for them, too, and I realize that absent the arrogance of most medical review boards and the ambition of prosecutors clamoring over each other’s backs looking for media exposure, help would be readily forthcoming. I wish those doctors nothing but the very best, and as such, as much as I almost don’t want to, all that I can advise them is to keep doing what they are doing now because they do absolutely have targets on their backs. To those ambitious prosecutors and the select arrogant medical “elite”, I wish them the same thing they wish – no, that they actually deal on me, say what they want – as much horrible and unending pain and misery as misfortune can deal on them by the absolute worst medical pathologies, disease and injuries that can that be visited upon them for as long as is humanly possible. That may be wrong, but it’s my wish.