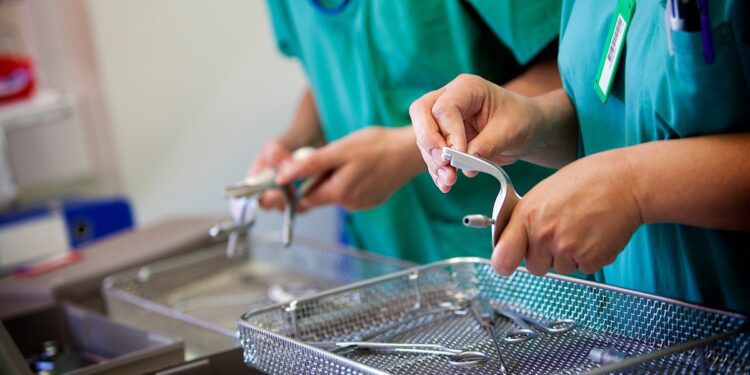
Surgical safety depends on far more than clinical skill in the operating room. Behind every successful procedure is a rigorously controlled system of cleaning, inspection, sterilization, and storage. Sterile processing standards influence surgical safety with infection prevention, regulatory compliance, and patient outcomes.
Moreover, Healthcare-associated infections (HAIs) remain a persistent concern in U.S. hospitals. The Centers for Disease Control and Prevention (CDC) estimates that approximately 1 in 31 hospitalized patients has at least one healthcare-associated infection on any given day. While HAIs arise from multiple factors, improper instrument reprocessing is a well-documented contributor. This reality makes sterile processing not merely a technical workflow, but a patient safety priority.
The Link Between Standards and Infection Prevention
National guidelines from organizations such as the CDC and the Association of periOperative Registered Nurses (AORN) outline evidence-based practices for decontamination, inspection, packaging, sterilization, and storage of surgical instruments. These protocols address variables such as cleaning chemistry, water quality, sterilization cycle parameters, and biological monitoring.
When facilities adhere to these guidelines, they reduce the risk of retained bioburden, sterilization failure, and cross-contamination. Even small deviations—such as overloading sterilizers, improper packaging, or inadequate drying—can compromise sterility and increase the risk of postoperative infection.
In this context, sterile processing standards function as both clinical safeguards and operational guardrails. They ensure that reprocessing departments operate consistently, even amid staffing shortages or rising surgical volume.
Equipment Design as a Compliance Factor
Standards do not exist in isolation; they interact closely with equipment design. Instrument baskets and other systems must allow adequate penetration of cleaning solutions and contact with sterilants. Poorly designed containment systems can obstruct sterilization cycles or retain moisture, increasing the likelihood of contamination.
Healthcare facilities often evaluate equipment based on durability and cost, but compliance considerations are equally critical. Features such as appropriate mesh sizing, electropolished finishes, and compatibility with automated washers can influence cleaning efficacy.
Documentation, Traceability, and Risk Management
Modern sterile processing departments rely on detailed documentation and tracking systems. Load records, biological indicator results, and instrument traceability logs provide both quality assurance and medicolegal protection. In the event of a suspected sterilization breach, accurate records enable facilities to identify affected instruments and patients quickly.
From a health policy perspective, compliance with reprocessing standards also affects accreditation outcomes and reimbursement risk. Regulatory bodies increasingly scrutinize sterilization practices during inspections, reflecting broader attention to preventable harm.
A Systems-Level Perspective on Surgical Safety
Sterile processing standards greatly influence surgical safety, but many frame protocols around checklists and intraoperative protocols. Yet preoperative processes—particularly instrument reprocessing—are foundational to safe care delivery. When consistently implementing standards, supported by appropriate equipment, and reinforced through training and documentation, they create a culture of accountability that extends into the operating room.
In an era of value-based care and heightened regulatory oversight, sterile processing is not merely a technical department in the background. It is a central pillar of patient safety infrastructure.